
Engineers are natural problem solvers. At Lehigh, the Center for Community-Driven Assistive Technologies (CDAT) is built on the idea that the most meaningful solutions emerge when engineering expertise is paired directly with lived experience. In other words, people facing accessibility challenges and those who support them help shape and guide the center’s work.
“Community members tell us the problems they face so we can design, develop, and translate the tools that will have maximum societal impact,” says CDAT director Vinod Namboodiri, a professor of computer science and engineering and the Forlenza Chair in Health Innovation and Technology in Lehigh’s College of Health (COH). Launched in 2025 as one of three new University Research Centers, CDAT brings together faculty, staff, and students to develop technologies that will improve life for people with disabilities.
“Starting with a community problem isn’t easy—any single faculty member may lack the skills to solve it,” Namboodiri says. “But that’s where our ability to work in collaborative, interdisciplinary teams makes a difference.”
Prior to the center’s launch, Namboodiri and his team held a workshop in 2024 to better understand the scope of local challenges. They invited participants from medical organizations like Good Shepherd Rehabilitation (a clinical and research partner of Lehigh), nonprofits such as the Lehigh Valley Center for Independent Living and the American Foundation for the Blind, senior living centers, and multiple school districts. Working together, they named three focus areas: Mobility and Access, Transitions, and Smart Spaces. Although CDAT is still in its early stages, projects in each area are already being defined—and in some cases, underway.
 Moving through the world
Moving through the world
Juan Aceros leads the Mobility and Access focus area. The associate professor of bioengineering, who also has a joint appointment at Good Shepherd Rehabilitation, specializes in pediatrics and develops ride-on toys and technologies that help children with disabilities better engage with the world.
“Our objective is to improve quality of life through mobility so that people can participate in the activities they enjoy,” he says.
Projects in this area include Mapping for Accessible Built Environments (MABLE), an ongoing initiative headed by Namboodiri that allows people with a range of impairments to use an app to receive turn-by-turn instructions while navigating indoor environments.
Another proposal involves a harness system for individuals unable to stand independently because of injury or stroke. The concept resembles a canopy that opens and locks into place, says Aceros. The harness could support a person’s body and enable them to walk.
“That person could then work, for example, behind a counter at a café,” he says. “Having that harness system allows them to be out in the world, engaging with people, and doing physical activity. It has the potential to be life-changing.”
That work builds on research Aceros launched earlier in his career, in which he and his team at the University of North Florida demonstrated that ride-on toys can have a measurable psychosocial impact on very young children with disabilities by enabling them to move through and interact with their surroundings. The devices resemble small ATVs and are adapted to each child’s needs.
For example, if a child has weak lower-body control due to spina bifida, the device may require standing to strengthen leg and core muscles toward the long-term goal of advancing from a wheelchair to independent walking. For children with more severe disabilities, the ride-ons can be operated by others and paired with helmets that support the head and encourage eye contact—an essential element of human connection.
The next step, Aceros says, is studying how the devices influence biomechanics, including gait and postural control, across populations.
“Some of the children who use these devices show significant improvements in mobility, posture, and communication, while others don’t,” he says. “So we’re embedding high-tech sensors in the toys to identify patterns in how they’re used and how that correlates with improvement. That data can help clinicians make informed recommendations—such as how often and how long a child should use the device—to maximize benefit.”
His team has already begun building a motion-capture lab at Good Shepherd. The space, which he plans to eventually relocate to Lehigh’s campus, will allow researchers to more precisely measure movement patterns and integrate those findings into the design of future ride-ons.
 A related project explores the integration of vibration therapy into ride-ons for children with little to no ability to move from the neck down. Vibration is commonly used in clinical settings prior to treatments like physical therapy, says Aceros, because it activates mechanoreceptors that boost muscles’ responsiveness and extend the effects of treatment. The toy will incorporate a supportive harness and vibration technology to stimulate core muscles.
A related project explores the integration of vibration therapy into ride-ons for children with little to no ability to move from the neck down. Vibration is commonly used in clinical settings prior to treatments like physical therapy, says Aceros, because it activates mechanoreceptors that boost muscles’ responsiveness and extend the effects of treatment. The toy will incorporate a supportive harness and vibration technology to stimulate core muscles.
“The vibration will strengthen their muscles, and we hope to see improvements in trunk control,” says Aceros. “For these children, even small gains in posture control can help prevent ulcers, reduce pain, and minimize pressure sores. We want to understand whether a ride-on like this can independently function as a therapeutic intervention. I believe it can.”
Such research depends on collaboration across disciplines, and CDAT will provide access to that expertise, says Aceros. It will also help attract students eager to work on problems grounded in real-world impact. “Students who gravitate to work like this want to see their energy and intellect translated into the community and into projects that matter,” he says.
Preparing for change
Another focus area, Transitions, centers on helping people with disabilities as they move through major life stages, such as from high school to college or from employment into retirement. It’s co-led by Lee Kern, a professor of special education in Lehigh’s College of Education, and Fathima Wakeel, an associate professor of population health (COH). One project involves developing methods that use augmented reality to simulate life in higher education for individuals on the autism spectrum.
“These students are used to a certain support structure and routine, so how do we prepare them for the changes to come?” says Namboodiri. “Solutions might include virtual reality wearables that immerse them in the sights and sounds of a college campus, or a large language model and chatbot that simulates events like a career fair. The goal is to give individuals—and their caregivers—a way to experience these transitions ahead of time and feel more confident navigating them.”
 Integrating tech in daily life
Integrating tech in daily life
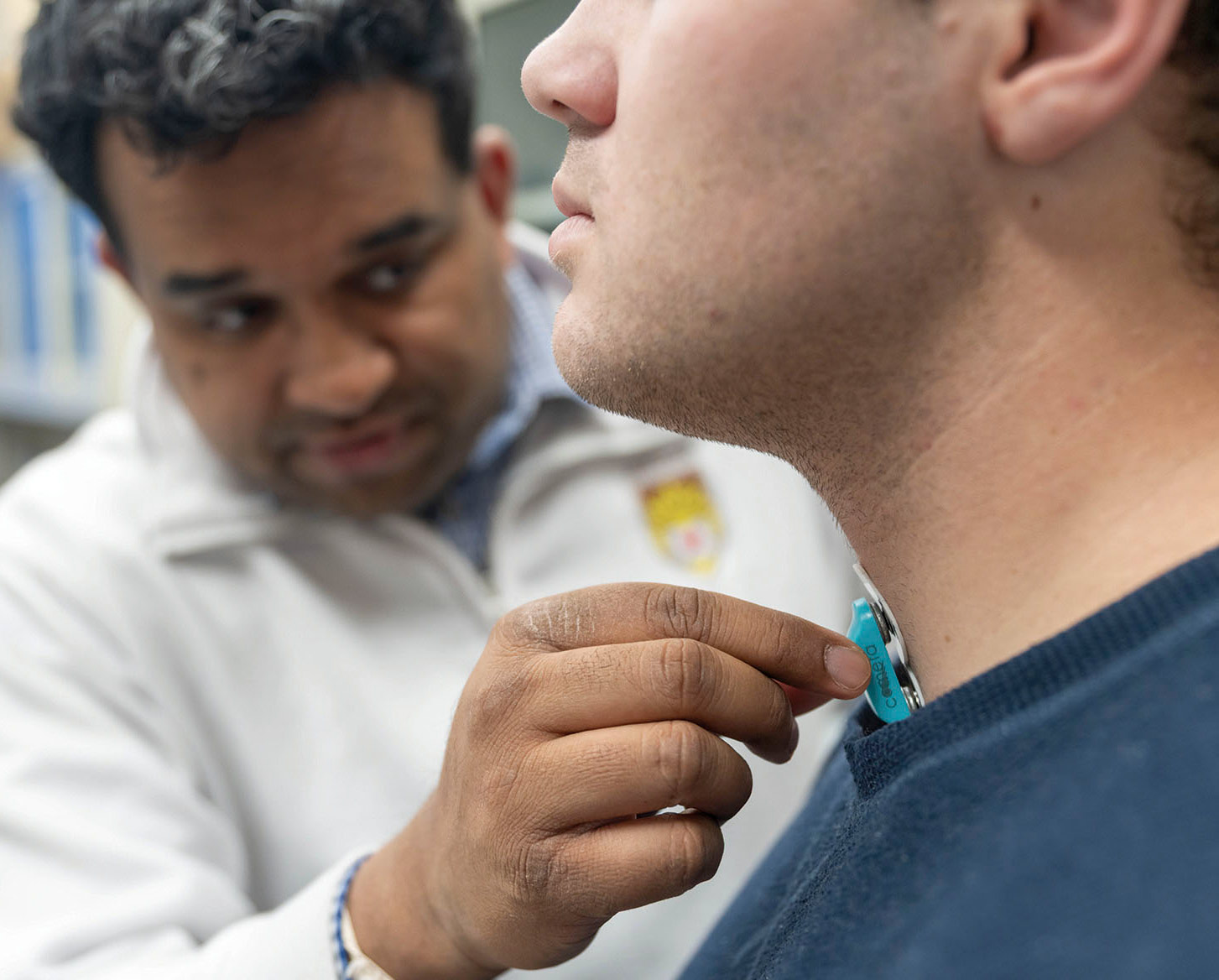
The third focus area, Smart Spaces, explores how technology can support people in activities of daily living. It’s co-led by Mooi Choo Chuah, a professor of computer science and engineering and an associate director of Lehigh’s Institute for Data, Intelligent Systems, and Computation (I-DISC), and Dhruv Seshadri (pictured), an assistant professor of bioengineering. Several projects have already received funding, including one focused on individuals with dysphagia (difficulty swallowing) and another on people with multiple sclerosis (MS).
In the dysphagia project, researchers are developing algorithms and placing sensors on the neck to measure the effort and frequency of swallowing. “Ultimately, we’re trying to quantify what therapists currently assess subjectively, using tools like perceived exertion,” says Seshadri. “We aim to provide objective data clinicians can use to better understand and tailor treatments to address dysphagia.”
Seshadri hopes to eventually pair the software with a device that integrates swallowing metrics alongside other vital signs, such as heart rate and body temperature, to assist with diagnosing related conditions. “Patients with dysphagia can develop aspiration pneumonia,” he says. “When food enters the windpipe, it can cause infection and trigger changes in respiratory rate, heart rate, and temperature. Given its life-or-death importance, we’re interested in the potential of swallowing as the next digital biomarker of disease.”
Seshadri’s team is taking a similar approach to quantifying muscle fatigue—which can lead to gait abnormalities and falls in people with multiple sclerosis—as a way to assess and improve therapy. Sensors will measure changes in muscle activity during standard rehabilitation exercises such as walking and sit-to-stand tests. Currently, fatigue is largely assessed through a patient’s self-reporting.
“We’re trying to provide the first quantifiable means of assessing rehabilitation outcomes in patients with MS,” he says, “so we can deliver clinically meaningful information to physical therapists.”
